CPS is still playing catch up on public health two years into the pandemic
CPS had little to no public health infrastructure when COVID-19 hit. When it turned to the city, it found a similarly strained setup.
By Sarah Karp, Becky Vevea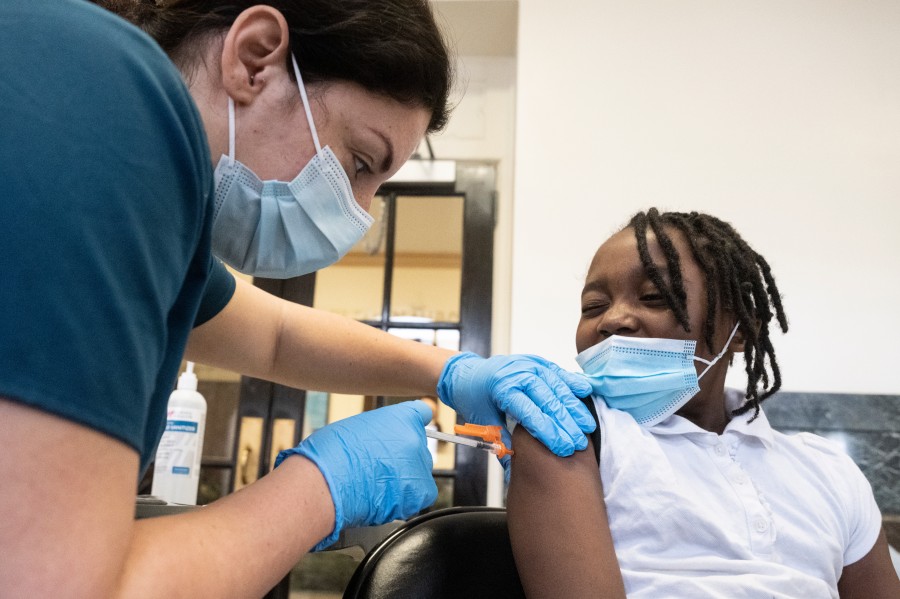

CPS is still playing catch up on public health two years into the pandemic
CPS had little to no public health infrastructure when COVID-19 hit. When it turned to the city, it found a similarly strained setup.
By Sarah Karp, Becky VeveaTwo weeks after COVID-19 vaccines were approved for children 5 and older last fall, Chicago Public Schools canceled classes, declaring Nov. 12 “Vaccine Awareness Day.”
The school district spent more than $7,000 on balloons, signs and cupcakes to encourage kids to get vaccinated that day. It also paid community groups $8,000 to watch children if their parents had to work.
Some 20,000 children got shots that day, the most for any one day.
It was a splashy move for a district that has been struggling all year to offer the pandemic protections it has promised.
Student vaccination rates vary widely across the school district, with some communities topping 80% while others are still below 15%. Both contact tracing and testing were slow to get started, with almost no testing in place when the school year began. Contact tracing teams are just adding school-based employees now and the district is only now gearing up to test 10% of students in each school. Some of these changes only materialized after a five-day standoff with the teachers union in January.
CPS CEO Pedro Martinez acknowledged last month that the district has been struggling.
“I’m asking the community to give us some grace because we’re learning,” he said in mid-January. “We’re not a health institution.”
The reasons for the delays and stumbles are many, but one stands apart: CPS had virtually no public health infrastructure when the pandemic began and little expertise to launch a massive public health response. With $2.8 billion federal funding, plus a grant from the Centers for Disease Control and Prevention, money has not been the main problem.
CPS’ officials note the school district has always provided health services to students, as outlined by federal, state, and local policy. And in 2012, it created the Office of Student Health and Wellness.
But that office has had a relatively small staff of mostly program managers and trainers. Nurses and social workers, who are focused on special needs students and are in limited supply, are not part of that office. One of the health office’s biggest pre-pandemic initiatives was incentivizing schools to create wellness teams and to have staff in schools trained in assisting students in things like daily diabetes management.
And when district leaders turned to the city’s department of public health, they found an equally stretched public agency that primarily relies on private health care providers. The department only had a handful of people to create and execute safety plans for all private and public schools and colleges across the city.

Testing and contact tracing
The most complicated — and problematic — element of the school district’s pandemic response has been its testing and contact tracing programs. Both are still struggling to deliver on promises made at the start of the school year.
Before school began, the school district pledged to provide weekly a COVID test to all students who wanted one. But for months the school district struggled, even as demand was low.
Since January, after the school district committed to testing 10% of students in each school in an agreement with the teachers union, the number of students signed up for regular testing has increased dramatically. As of Monday, 94% of all schools have 10% of students signed up.
But getting timely results remains an issue.
Nearly 10 months ago, in April 2021, the city gave the school district $60 million in federal COVID-19 relief funds for surveillance testing in schools. The city could have run the testing program itself, but officials said they chose to hand it over to CPS because the school district already had a testing program in place. They also said the school district had significant expertise within its Office of Student Health and Wellness.
But at the time, the school district’s surveillance testing program was small compared to what it would need to stand up going into the 2021-2022 school year.
Over the summer, 33 companies submitted bids to run CPS’ testing program, including Walgreens, the University of Illinois’ covidSHIELD test and a host of labs. CPS ultimately chose Massachusetts-based Thermo Fisher Scientific for the $60 million contract.
The rollout on CPS’ end has been rocky since the start. There have been numerous reports of adults tasked with administering the tests failing to show up at schools, and sign-ups were slow for months, at least in part because the process of enrolling students in testing was so cumbersome.
There also appears to be capacity issues. Parents have complained about test results taking days to be returned, rendering them useless. In addition, the school district paid Thermo Fisher $8 million to send 150,000 tests home with students over winter break to test before returning after the holidays. But the tests piled up at dropoff boxes, and most did not arrive at out-of-state labs in time to be analyzed. More than 60% of the tests returned couldn’t be analyzed.
CPS said it holds vendors accountable and that Thermo Fisher agreed to credit the district $1.35 million toward future testing costs and services.
In choosing a testing company, the school district assessed 10 factors and put the greatest weight on meeting CPS’ IT requirements. Thermo Fisher tied with three other companies for the top score in that area.
The school district said the IT component referred to the vendor’s platform to collect, analyze and present the data — specifically the test results — to staff and families. “For a district that serves more than 330,000 students, this was important but not the most important factor in our evaluation,” the school district said in a statement to WBEZ.
Capacity to undertake the program was not weighted as heavily as IT by CPS. And that was an area where Thermo Fisher did not score as well. It ranked 23rd out of 30 companies, according to CPS bid documents obtained by WBEZ. At least one reviewer questioned the company’s plan to use already-stretched CPS staff to perform testing or to make it self administered.
The school district said eight factors, including capacity, as well as data collection and reporting, vendor qualifications and references, were key considerations and when grouped together, accounted for significantly more than IT. When the points earned for each of the 10 factors were added together — those eight plus IT and pricing — Thermo Fisher’s proposal ranked in the bottom of the top five.
But when Thermo Fisher representatives sat for an interview and an oral presentation, they earned higher scores in several categories, including capacity, especially from one reviewer.
After the interview, Thermo Fisher’s score shot to the highest among the five finalists, sealing the deal for them.
But many parents have been unhappy with how the testing program has gone.
“Testing was something that I was counting on to keep my daughter safe this school year,” Nicole Granacki, a CPS mom of a preschooler, said in late January. “It has been a big disappointment.” Granacki said results were taking five days to come back, which left students vulnerable to being exposed.
A spokesperson for Thermo Fisher did not address delays in testing and the difficulty in building capacity, but said the company has the capacity to process 20 million tests per week and has lab partners across the country. It defended the ReadyCheckGo testing program in use in CPS.
“Thermo Fisher Scientific’s depth of capabilities and the expertise of its partners are key factors that have enabled the ReadyCheckGo program to scale with the evolving needs of its customers across the United States,” the company said in a statement. “Most recently, we worked closely with our partners to successfully double the program’s capacity to meet testing, staffing and logistics demand that resulted from the recent omicron variant surge.”
Slow contact tracing has also been a major issue for Chicago Public Schools.
CPS started the academic year with just 13 contact tracers on staff and quickly found they did not have enough staff to do the investigations and to reach out to families. Some parents weren’t informed of possible exposures for days, even a week after the district was notified. The school district ramped up to 48 contact tracers as of Dec. 31 and signed onto an idea from the Chicago Teachers Union to pay school-based teams to do contact tracing.
When the program was getting started, CPS and the city Department of Public Health discussed which institution should support contact tracing, according to CPS. Ultimately they decided CDPH would provide guidance but CPS would be in charge of the staffing, training, and doing the actual contact tracing.
CDPH’s focus isn’t on direct service. Its primary role is to coordinate private providers, which is what it did in setting up its own contact tracing program at the start of the pandemic. The city awarded $56 million to an outside group to coordinate the contact tracing work with community groups, an effort that took months.
New York City’s public school system has a different model for COVID-19 testing and contact tracing. Its “Test and Trace Corps” is led by the NYC Health + Hospitals, a huge public hospital system, and works in collaboration with the New York City’s department of public health.
The Corps has also partnered with community agencies and also hired Americorp workers. Dr. Ted Long, who runs it, told WNYC in an interview that by working with people in communities who know the families and the dynamics, the process goes more smoothly.
The Corps, though, have also been criticized by parents who say they aren’t getting information about exposures quickly enough. But Long says that 92% of families get notified within 24 hours.
After all the work setting up testing and contact tracing, CPS and other school districts will soon have to decide if continued testing is still worth the effort.
Dr. Larry Kociolek, a pediatric infectious disease doctor at Lurie Children’s Hospital, said testing helps when a virus is spreading rapidly in a community. But it’s not as valuable when cases are low.
“It’s logistically challenging, and at some point it becomes not very beneficial,” Kociolek said.

The vaccination race
There’s wide agreement that the way forward for Chicago Public Schools is to get kids vaccinated.
The Chicago Department of Public Health has experience with vaccinating children for diseases such as the flu. This helped give CPS more of a head start in responding to the pandemic compared to contact tracing and testing. But neither CPS nor CPDH have an army of nurses or other staff they can deploy to schools for COVID vaccinations.
Currently, CPS has about 490 nurses focused primarily on special needs students, but as their ranks are growing they have more time for the general student population. A school nursing manager has only recently been hired in the Office of Student Health and Wellness. The city employs 65 nurses, half as many as it did a decade ago. Last year, the city also spent millions contracting with a for-profit company to provide temporary nurses to staff vaccine clinics and testing centers.
“Our health care system overall tends to be very privatized and individualized,” said Dr. Allison Arwady, the city’s public health commissioner. “And I think we have seen in COVID, that there are limits to that.”
She said the approach of having a government that does testing or providing the vaccine has not been the norm in Chicago.
Arwady’s department is focused on coordinating care, not delivering it. CDPH works with a big network of federally-qualified health centers, large hospitals and for-profit health care companies where Chicagoans primarily get their medical care. These providers have been vaccinating teens since last summer, and children five and older since November.
Separately, the school district has hired companies to provide vaccinations at its events.
The school district and the city say they are doing their best to get as many shots in arms as possible. Still, the process has been slow, as it has been nationally. Vaccination rates for CPS teens have stagnated at around 54%. For children 5 to 11, only 22% are fully vaccinated, according to CPS. The rate for CPS’ youngest student students lags behind the 37% citywide average for all 5- to 11-year olds.
On a cold January morning recently, the door to the auditorium at Park Manor Elementary school in Auburn Gresham was ajar. A sign gave notice that COVID-19 vaccines were being administered inside.
If any school was going to have a strong vaccination event, it would likely be this one.
Prior to winter break, the school had so many cases that, according to staff, most classes were remote. The Chicago Teachers Union held multiple press conferences at the school where staff rallied to ask for more support.
But inside the auditorium, there were only a handful of students. Kimberly Safford was sitting behind a folding table waiting to administer a shot. She works for an independent contractor that runs some of the school-based events.
Safford said many of these sessions are “up and down,” but she considered Park Manor’s event “pretty successful” with 20 adults and children getting vaccinated. About three students got shots without their parents present, she said.
As of Jan. 18, 22% of Park Manor students had received at least one shot. That’s below the citywide average, but higher than the seven other elementary schools in the area. Even at the area high school, Hirsch, where students had since summer to get vaccinated, only a quarter of students have received at least one dose. In the surrounding community, just over 63% of adults are fully vaccinated, which lags the citywide rate of 76%.
Vaccination events like the one at Park Manor ramped up after the CTU work stoppage in early January. Most are during the week, from 10 a.m. to 1 p.m. Parents can come in, but they are able to give consent ahead of time.
CPS also has 33 school-based health centers for students and in some cases, anyone in the community. Twenty four of them are offering COVID-19 vaccinations. All are run by private health care providers and provide broad primary care services. Most are offering COVID-19 shots by appointment.
“We didn’t just pop up a vaccine clinic for a day and then leave,” said Dr. Mark Minier, medical director of pediatrics and school-based health services for Esperanza Health Centers, which runs the school-based health center at Marquette Elementary. “[Patients] know who we are.”
Vaccine appointments during the work day can be challenging for parents. That’s why the Department of Public Health also has vaccination clinics at City College of Chicago campuses on Saturdays and Sundays.
Mayor Lori Lightfoot also touts the city’s at-home vaccination program.
“What we’re seeing is when we go into homes, we get the opportunity to vaccinate every single family member who’s eligible,” Lightfoot said.
As of Jan. 25, 6,373 children ages 5 to 17 had been vaccinated through the at-home program, public health department officials said. That’s out of the more than 100,000 children vaccinated citywide.

City and school district officials insist the problem isn’t about access.
“Our challenge is persuasion,” said Dr. Ken Fox, who resigned last month as CPS’ Chief Health Officer. “How are people best convinced that the vaccine is safe and effective? What would make that message most compelling?”
In a presentation to the Board of Education, Fox said the school district plans to launch a campaign to tackle hesitancy in addition to the videos, messages to families and other efforts underway.
This comes months after the vaccines became available. Like much of the pandemic response, the strategy is still being developed.
Sarah Karp covers education for WBEZ. Follow her on Twitter at @WBEZeducation and @sskedreporter.
Becky Vevea covers city politics for WBEZ. Follow her @beckyvevea.
