Sara Navin has gotten tested for COVID-19 three times now. And, each time, the process has been a surprisingly pleasant experience.
“I just sign up on the city’s free website where you don’t need insurance or any symptoms to make an appointment,” she said. “It’s really easy.”
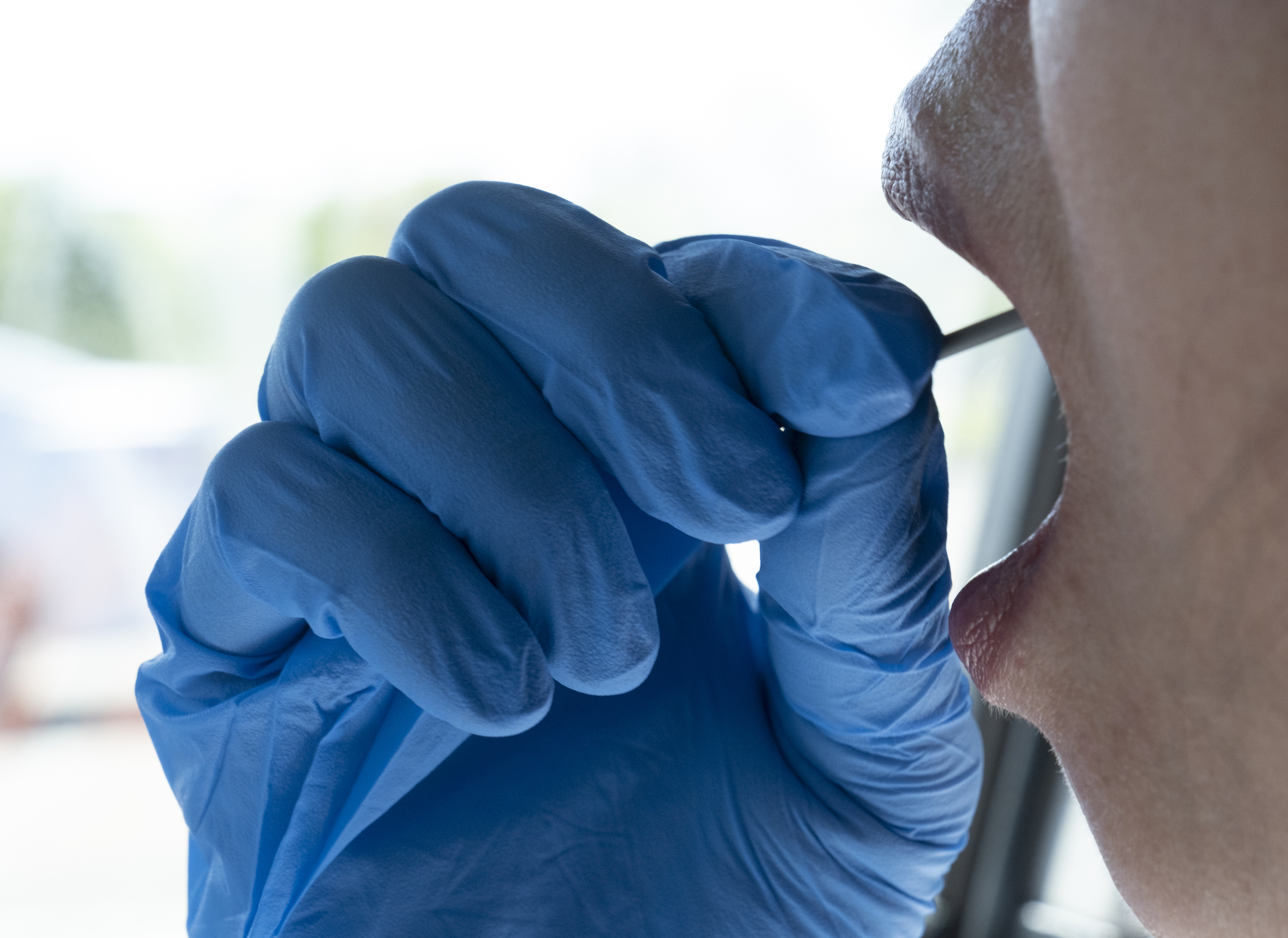
Part of that ease, Navin said, was the painless sample collection process. She simply sat in her car, coughed three times, swabbed her mouth for 20 seconds and then sealed the swab in a vial.
This was a relief since she’d heard horror stories from friends about invasive sample collections — called nasopharyngeal swabs — that involved getting long plastic sticks jammed up their nose.
“Most of the other people I’ve talked to have gotten that [deep] nasal swab,” she said, “And so I was wondering why city of Chicago sites were doing the mouth swab and if there was any difference in the accuracy of those tests.”
We’ve heard similar questions from other Chicagoans who wonder why they were subjected to the uncomfortable nasopharyngeal swab (NPS) — affectionately referred to as the “brain poke” — while their friends got to administer their own mouth or nasal swabs. Many assumed the less invasive collection methods must not be as good, and they wanted to know why there was such a wide variety of methods instead of one standard.
We took these questions to doctors, researchers and health officials and learned that pandemic shortages have forced healthcare providers to use several collection methods in recent months.
But we also discovered some good news for people like Sara: Emerging research suggests that self-collected mouth and shallow nose swabs can be nearly as good, or better, than nasopharyngeal samples at detecting COVID-19. In fact, in late April, federal health authorities officially removed their preference for the use of NPS in COVID testing. And, beyond accuracy, the non-NPS methods offer some important advantages when it comes to ramping up testing to fight the virus.
The “brain poke” method has pros and cons
Still, most microbiologists and pathologists we talked to maintain their preference for nasopharyngeal samples as a first choice.
“The gold standard is the nasopharyngeal swab,” said Karen Kaul, chair of the pathology and laboratory medicine at NorthShore University Health System. “The COVID virus, like other viruses including the flu, likes to live in the nasopharynx and so that is the best place to go.”

This is why you still primarily see NPS collection at big hospitals such as Northwestern Medicine, Loyola University Medical Center and NorthShore University HealthSystem. But Kaul said they’re all looking into alternatives because NPS has some major drawbacks right now.
"In order to collect [using NPS] you need an appropriate supply chain of swabs which is one of the problems we’ve been dealing with,” she said. “And it also requires a bit more training than other collection methods."
An even bigger problem may be the danger to healthcare workers who have to wear PPE and change it often, because when you put a stick up people’s nose, they “sneeze and cough, [creating] a risk of exposure there,” Kaul said.
On top of that, some patients swing their arms, swat away the swab or even accidentally hit healthcare workers as they involuntarily react to the “brain poke.”
So, in recent months, medical professionals have turned to alternate collection methods including throat swabs, shallower nasal swabs and mouth swabs.
“At University of Chicago, we started collecting [samples] from the front of the nose rather than the back of the nose [using NPS],” said Dr. Kathleen Beavis, the medical director of Microbiology and Immunology Laboratories at UChicago Medicine. “We wanted to do that for a few reasons and one of them was comfort to the patient … so now most specimens are collected that way at University of Chicago.”
Beavis said front-of-the-nose samples (also called anterior nasal sampling) are proving just as accurate for them and they will soon move to allow patients to collect their own anterior samples that way.
The quality of those samples was also tested by researchers in a small study at Stanford led by Dr. Yvonne Maldonado. Researchers found that self administered nasal swabbing produced good and sometimes better results than NPS samples gathered by health workers.
Mouth swab tests are convenient and may be more accurate
But what about the mouth swab tests that Sara and hundreds of thousands of other Chicagoans have been taking at free city sites for more than two months?
Ann Wyllie, associate research scientist at the Yale School of Public Health, looked at results from 142 patients and discovered something surprising: Among her subjects, mouth swabbing performed as well and in two cases better than nasopharyngeal swabbing.
Two of her subjects had been asymptomatic healthcare workers infected with COVID-19. The mouth swab test detected the virus but the NPS test did not.
“So that is when I thought, ‘O.K. we might have something here,’” Wyllie said of the unexpected result.
Wyllie’s study is still in the pre-publication stages, but she said she’s received “encouraging” feedback from peer reviewers and is gathering more data.
“We’ve updated the data set twice now and doubled the sample size and the findings are holding true,” she said.
A microbiologist by training, Wyllie said she was drawn to the topic because her PhD research examined the accuracy of saliva sampling in detecting a strain of streptococcus infection. Knowing that this might make some think she has a pro-saliva bias, Wyllie enlisted the collaboration of 49 other Yale scientists on the study.
Currently, Wyllie is also working on a way to accelerate the process by skipping a step called RNA extraction — where you pull out specific genetic material from the sample — and go straight to testing the whole saliva sample. She and her colleagues recently submitted a protocol for that faster process to the US Food and Drug Administration for approval. And they have an unlikely collaborator on the project: professional basketball.
“We are currently validating that method in partnership with the NBA to see how this also works for detecting [COVID-19] in asymptomatic individuals,” she said.
Chicago launches free mouth swab testing
This is good news for Fred Turner, the 25-year-old founder of Curative Inc., whose team developed the oral fluid mouth swab tests that are used by all of Chicago’s city-run community sites, as well as municipal testing centers around the country. His company had been working on sepsis diagnostics when it turned its focus to COVID in March as the scope of the pandemic became clear. So, why focus on mouth fluids?
“When we were evaluating different sampling methods back in March … one of the key criteria was that the country would need to screen millions of people every day so it had to be scalable,” the British native said. “And when you look at nasopharyngeal swabs, they are hard to scale. So we looked for a self-collection method that was easy to self administer whilst still being accurate.”
And that method was Curative’s particular protocol for mouth swabbing, which Turner is quick to point out is unlike other mouth swab or saliva samples being tested across the nation.
“Our method is an oral fluid swab test which means the individual first coughs three times,” he said. “The idea there is that the coughing releases virus in the lungs that gets caught in the saliva so that when you are swabbing the inside of your mouth and around your gums you are getting viral samples both from the lungs and upper respiratory tract as well as virus that would be in the saliva. So you are getting this two site sampling with a single swab.”
This protocol impressed officials at the Chicago Department of Public Health for many reasons — especially the self-collection aspect.
“It limits the potential exposure to the person helping collect the specimen and it cuts down on the amount of PPE needed for the people staffing the sites,” said Jennifer Layden, Chicago’s chief medical officer. “The other element is that it was essentially a self-contained kit which has the swab and the little vial all in one bag.”

And, to supply the kit, Curative Inc. sources equipment outside of the strained supply chains used by other testing protocols.
“This way we didn’t have to compete with or tap into resources that our clinical partners are using,” Layden said.
Curative’s test received emergency use authorization from the FDA in mid-April, and by mid-May, Chicago’s Department of Public Health had launched four sites using the protocol. Today, it also uses them in 50 mobile sites that travel around the city where needed, Layden said.
How to register for free testing at Chicago’s community testing sites
- Sign up for a test here. Any Chicagoan, with or without symptoms, may register. You’ll be asked questions about recent exposures and required to give an email address.
- Once approved, you’ll receive an email with a link to select a time and location among the city’s four sites and be given an appointment number.
- Show up at your scheduled time: Bring your appointment number and do not eat, drink or chew gum at least 20 minutes before your test. (Most arrive by car but there is a tent for non-drive up patients near the entrance).
- An attendant will stick a Post-It note with your appointment number on your car window; at the next station, you’ll receive a test kit packet slid through your window (open just two inches). You’ll move to the next station, where you’ll be instructed (again through the window, now closed) on how to administer the test to yourself: Cough three times, swab for 20 seconds, insert the sample into a vial, and shake.
- Drop the vial into the test kit packet and deposit the whole thing in a bin a few yards ahead. Your kit will be sent that night to labs in either California or Washington DC depending on which has the capacity to process that day, according to Curative Inc. CEO Fred Turner. Your results will be delivered via email — the readers we polled all say they got theirs back in 48 hours or less.
By mid-July, Layden said, the sites, staffed by workers from CORE (a community action nonprofit founded by the actor Sean Penn), had collected more than 46,000 tests. She said they will continue running the sites for the foreseeable future based on community need, which is reassessed regularly.
In some cities the Curative tests are billed to insurance, but in Chicago all tests are free to the patient. Layden said the city uses federal funds from the CARES act and the CDC to pay for the test but does not have exact figures on how much an average test costs.
Turner said his company’s clinical trials have found their oral fluid collection method to be 90% accurate in detecting COVID-19. By contrast, he said, the same trials showed NPS to be accurate 79% of the time. His methodology is explained in Curative’s emergency use authorization summary on the FDA site.

So, which test is best?
Microbiologists we talked to say they are impressed with the improving alternate technologies but that they still believe nasopharyngeal collection is the gold standard, even if it presents challenges at this time.
Just five months into the U.S pandemic, researchers are still working with relatively small data sets and say that different protocols and samples from patients at different levels of infectiousness are understandably showing slightly different outcomes.
But one of the largest studies, conducted by researchers at the University of Washington and United HealthGroup in Minnesota, found that three collection methods (front of nose, mid nose and tongue) all performed well against NPS, even when patients took the samples themselves. All three alternative methods detected the virus when NPS didn’t in a small number of cases.
“I think we’ve got lots of little pieces of the puzzle, and we are trying to make a clear picture out of something that is still pretty pixelated,” said Amanda Harrington, director of the microbiology lab at Loyola University Medical Center. “It’s not like we have one standarized approach to compare against, and everyone is using a different tool so I don’t know if I could compare my approach to my neighbor’s.”
In the end, though, she thinks Sara doesn’t have much to worry about.
“If you’re asking if we can use alternate collection devices and are they adequate to detect COVID, then by and large the answer is yes,” Harrington said. “The most important thing is for people to get tested.”
(Note: Illinois’ free testing sites also use self-collected samples that patients collect from their nose. IDPH officials did respond to questions about how many tests they have done, who is currently staffing the sites or what their average turnaround time is for results.)
More about our questioner
Sara Navin grew up in Evanston and now lives in Chicago. She recently earned her master’s degree in public health and epidemiology and will start a research job at the University of Chicago this fall.
When she heard the answer to her questions about the city’s mouth swab testing, she was encouraged.
“Even though we don’t have a ton of data, it’s good to know that there are at least some encouraging smaller studies,” she said. “I would feel secure going and getting tested there again.”
She also thinks it makes sense that the city’s testing program would turn to methods that use fewer resources and leave people with a better experience that they might recommend to friends.
“Every time I’ve gone, it has been really easy and a good experience,” she said. “One time it was even in a park where there was a taco truck and music and voter registration. I have definitely been talking it up to people.”
When she’s not working or studying, Sara said she likes to ride her bike and swim in the lake.
“I can’t wait for Chicago beaches to reopen again,” she said. “I feel like it's way safer than indoor dining.”
Until then, she will be enjoying bike rides around town — sometimes even to COVID testing centers.
Monica Eng is the reporter for WBEZ's Curious City. You can write to her at meng@wbez.org.
Correction: A previous version of this story misspelled Karen Kaul's name.



